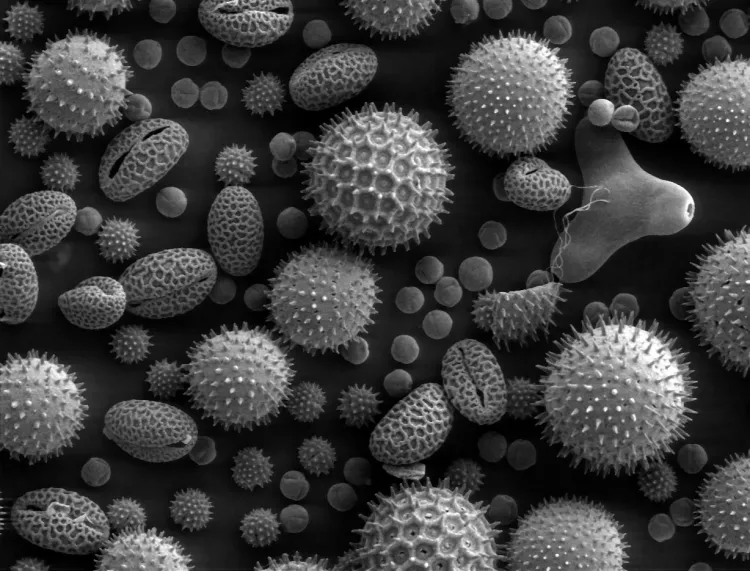
Asthma is a respiratory condition that affects 3-8% of the general population, thus also divers or would-be divers. It is defined as an increased responsiveness to the lower airways to multiple stimuli.
Contributed by
This increased responsiveness may be episodic and during such asthma attacks the brochi and brochioles will become inflamed and constrict and lined with mucus. This airway narrowing causes symptoms such as wheezing, shortness of breath, chest tightness, and coughing. The effects may range from mild without limitations of the patients’ activity to severe and life threatening. At times this obstruction may persist for days or weeks and it is called status asthmaticus.
Two types
There are two types of asthma: Extrinsic asthma and intrinsic asthma. Extrinsic asthma is when the asthmatic attack is triggered by an external cause. This form of asthma occurs in individuals who are termed as atopic. They also have associated eczema and hay fever. Intrinsic asthma is when no precipitating agents can be identified to bring on the attack. This form of asthma often occurs in middle age and patients may have negative allergic histories but develop bronchospasm after a respiratory tract infection. However, at times, there may be a history of childhood asthma in these individuals.
Attacks
Asthma may be triggered by a whole range of different factors. An asthma attack is based on non-specific hyperirritability of the Tracheobronchial tree but the mechanisms are not entirely clear. It has been postulated that the initiating stimuli activates a variety of chemicals that takes effect on the airway smooth muscle and blood vessel (capillary) permeability resulting in an intense local reaction. This may then be followed by a delayed (chronic) reaction. This latter response results in recruitment of more “inflammatory cells” to the site of injury. These then liberate a variety of chemicals compounds at the injured site which then result in more damage to the tissues.
All of which produce a wide spread effect within the tracheobronchial tree resulting in bronchoconstriction – constriction of the airways.
This bronchoconstriction results in the patient’s entire pulmonary function being compromised. Such that the rate of forced exhalation being lesser than the predicted level. Furthermore there will be an increased air trapped within the lung and this further compromises lung function. Besides, in asthmatics there may be other associated changes like heart (right ventricular hypertrophy) and lung (pulmonary hypertension) problems
Diving and Asthma
Asthmatics account for about 1% of the population of divers. But in countries where medical questionnaires and examinations are required prior to diving, the percentage of asthmatic divers are less.
The ocean environment exposes the diver to a variety of constantly changing stressors many of which may trigger asthma. The resulting bronchoconstriction and increase in airway resistance heightens the risk diving related disorders - in particular pulmonary barotraumas such as embolism. Also as asthmatics breathe with higher than average lung volumes (due to some degree of gas trapping), there is a theoretical increased risk of lung expansion injury during ascent. Most asthmatics are also under treatment with medication like bronchodilators.
This provides relief to some but not effect the entire airway. Hence, they may enable the asthmatic diver to descend easily but are less effective towards the end of the dive and also when a rapid emergency ascend may be required. More importantly, bronchodilator medication has a potential of causing an arrhythmic effect on the heart and is a potentially hazardous medication in the undersea environment.
As diving takes place in a dynamic environment with changing weather, tides, currents etc all divers will inevitably encounter situations requiring strenuous exercise at some point. Should an asthmatic attack be precipitated at such a time it would be detrimental. Consequently it will be ill advised for those with exercise induced asthma to enroll in or proceed with their diving course. Besides, in some asthmatics, seawater itself may also provoke an asthmatic attack. Thus the procedure of doing a hypertonic saline challenge test on asthmatics is able to within reasonable doubt rule out this aspect of asthma provocation.
Trigger factors in diving:
- Exertion – ie from swimming against current, equipment drag or being overweight
- Breathing cold and dry hyperbaric air, which increases dehydration of the airways
- Hypertonic Saline. Inhalation of seaspray or water (bubbling or leaking regulator)
- Breathing resistance (increased gas density , regulator problems, and low air supply
- Hyper ventilation and hypercapnia
Can I dive or not?
A number of factors have to be weighed and that can only be done in consultancy with a doctor. While asthmatics with normal airway function have similar risk as non asthmatics, in general asthmatics do have a higher susceptibility to pulmonary barotrauma. A study done on diving deaths showed that asthmatics accounted for 9% of diving deaths while asthma being a contributory factor to the death was seen in 8% of the deaths. Most of the deaths were in practically physically fit young men
Risk points:
- Risk of air trapping predisposing to pulmonary barotrauma
- Risk of an acute bronchospasm whilst diving and predisposing to pulmonary barotrauma and subsequent drowning.
- Risk of acute bronchospasm whilst diving and reducing exercise tolerance while on the surface and underwater.
- Risk of Decompression Illness in a diver who has recently taken a bronchodilator drug.
Can it be managed?
Asthma is managed through drugs and an asthma management plan. There are 2 types of medication in the treatment of asthma - relievers and preventers. As their name implies, relievers are used to treat the acute attack – so as to relax the smooth muscles. Some relievers also reduce the swelling and the mucous production. Preventers on the other hand help to prevent symptoms from arising thus stifling the degree of the allergic response to the precipitating agent.
Testing the severity of asthma and the likeliness of attacks includes a number of physical tests to see how the lungs react to a number of stressors. First of all the patient is put on an exercise bike for 5 mins at a load that corresponds to swimming 1 knots. The lung functions are measured before and after. It is also tested how the lungs reacts to inhaling saline and methacholine sprays. ■